Introduction
In healthcare, technological advancements are a great way to solve problems and create new opportunities, they also introduce new streams of research to the field due to their effect on patient outcomes. The proliferation of these technologies, notably telemedicine, is likely to make a turnaround in delivering healthcare services and patient-doctor communications and consequently influence health outcomes. This study demonstrates the analysis of the research work to determine the implementation of telemedicine in healthcare operations. The research focuses on the effect of telemedicine on patient outcomes inside healthcare facilities. The center of the analysis is to discover how telemedicine interventions can affect several aspects of patient care. The determinants to compare for the effectiveness of telemedicine in the healthcare sector are outcomes, patient satisfaction, healthcare utilization, and overall quality of care.
Hypothetical Analysis
Patient Satisfaction
One of the hypothetical analyses involves examining patients’ ratings between telemedicine services and traditional face-to-face healthcare encounters. For example, hypothetical situations might propose that patients who adopt telemedicine do so because of the comfort and time-saving attributes, reduced travel, and increased access to doctors (Aashima et al., 2021). Descriptive statistics were used to summarize patient satisfaction scores. The descriptive statistical analysis used to determine the impact of telemedicine is the comparison of the mean percentages of satisfied patients for a specific healthcare institution. The description of the analysis provided insight into the role of telemedicine in the healthcare department. This is depicted in a graph comparing telemedicine and the traditional method over time.
Clinical Outcomes
The analysis also includes evaluating the influence of telemedicine on clinical outcomes. Health improvement was considered when determining the impact of technology on the outcome (Merrill et al., 2022). It is essential to identify the impact of telemedicine technology on the participants. The analysis will focus on disease management. The healthcare providers will be interviewed on their perception of telemedicine’s impact on disease management. The comparison between the records of the interventions in disease management will be critically analyzed and evaluated. This analysis will employ the ANOVA test as the statistical tool to evaluate the impact of telemedicine on disease management. Some considerations will be taken into account before applying the inferential analysis. For instance, evaluating the effectiveness of the demographic selection and the participant’s health status is essential.
Healthcare Utilization
A general hypothetical perusal can be used to analyze the trend of healthcare utilization, including the number of hospital admissions, emergency department visits, and overall healthcare expenditures. Role-playing scenarios such as early intervention, better access to preventive healthcare, and better management of chronic conditions may mean reduced utilization of the healthcare system overall. Descriptive statistics offer a better understanding of the current use indicators, such as the mean number of inquiries per patient and the rate of admission reduction in telemedicine user groups. The evaluation findings will highlight telemedicine’s effects on health services utilization. Lowering the average cost after the deployment of the telemedicine tech implies that the technology is effective in promising healthcare utilization (Eze et al., 2020).
In this study, which is conducted under hypothetical conditions, we will uncover the following aspects: patients’ satisfaction, clinical outcomes, and modification of healthcare management with the applications of telemedicine innovations. Even though the research would not be conducted concretely, it could be analyzed through fictional situations and will show the predicted results and patterns.
Demographic Analysis
The overriding consideration in assessing the effects of telemedicine on healthcare access and quality is the demographic makeup of the participants enrolled in the study. This study will entail 300 participants, including 75 healthcare providers and 225 patients from 5 healthcare institutions. The following are the characteristics of the populations that will be used in the study.
Age: The participants included in the study were from different ages. There were both young and old individuals. The ages of the participants ranged from 20-59 years old.
Gender: Among the subjects may be females and males, with no discrimination based on their gender.
Socioeconomic Status: Participants come from different social statuses, which consist of those who are from low, middle, and high-income levels.
Geographic Location: This research might include participants from urban, suburban, and rural areas to ensure that different geographical locations are represented.
Gathering demographic data is imperative so that the study findings are applicable and are worth representing across the different demographic groups. This data can offer perceptions of how telemedicine impacts various population segments differently and will enable the preparation of specific measures to deter certain problems.
Descriptive Statistics
The descriptive statistics will help summarize the patient satisfaction rating scale. Mean scores for satisfaction were computed and compared between telemedicine and traditional face-to-face meetings. Hypothetical scenarios probably would be associated with higher mean satisfaction scores of telemedicine due to convenience, time-saving, minimized travels, and increased number of physicians available. Descriptive statistics also analyzed clinical variables such as health status improvement or illness recovery. The evaluation of the various aspects of the patient outcomes was compared with traditional care. Furthermore, descriptive statistics were used to give the size of healthcare utilization, including the mean number of telemedicine consultations per patient and admission rates. Hypothetical situations may predict that hospitalization and emergency department visits will be lower in telemedicine users, which, in turn, could bring down total healthcare expenditures.
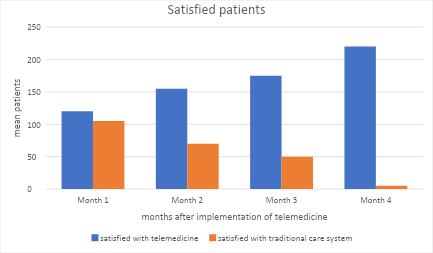
Figure 1: Patient satisfaction means comparison
From the above graph (figure 1), it is evident that the mean number of satisfied patients with the implementation of telemedicine increases over time. The low satisfaction in the first month could be due to the resistance from the patients to accept the implemented technology.
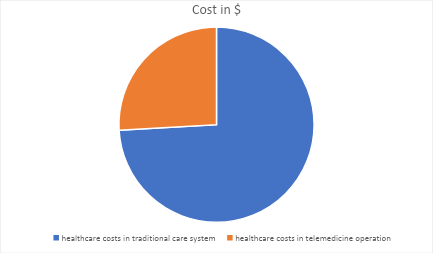
Figure 2: Pie chart comparing the costs
Implementing telemedicine plays a crucial role in ensuring that the application of healthcare services is effective. It is essential to ensure an effective application of telemedicine technology to reduce healthcare costs, as the chart above indicates.
Inferential Statistics
ANOVA test is the tool that was employed to evaluate the application of telemedicine to disease management across different groups. The test was used to compare the mean improvement scores through disease management among patients with varied levels of telemedicine usage. Through the ANOVA analysis, researchers can conclude whether there is any statistically significant disparity between telehealth and conventional care groups.
| pre-implementation | Post-implementation | ||
| institution 1 | 50 | 80 | |
| institution 2 | 45 | 76 | |
| institution 3 | 55 | 85 | |
| institution 4 | 64 | 88 | |
| institution 5 | 56 | 86 |
| Anova: Single Factor | ||||||
| SUMMARY | ||||||
| Groups | Count | Sum | Average | Variance | ||
| pre-implementation | 5 | 270 | 54 | 50.5 | ||
| Post-implementation | 5 | 415 | 83 | 24 | ||
| ANOVA | ||||||
| Source of Variation | SS | df | MS | F | P-value | F crit |
| Between Groups | 2102.5 | 1 | 2102.5 | 56.44295 | 6.84E-05 | 5.317655 |
| Within Groups | 298 | 8 | 37.25 | |||
| Total | 2400.5 | 9 |
The ANOVA analysis above compares the pre and post-implementation of telemedicine and the rate at which the staff manages the disease. From the analysis, it is evident that there is no significant relationship between the pre and post-implementation of telemedicine. The significance is lower than the p-value of 0.05, which indicates that there is no significant relationship.
Research Data Management (RDM)
Understanding Institutional Policies: Researchers must get acquainted with the institutional guidelines and laws on data management. It implies the knowledge of data storage, sharing, and preservation guidelines given to the establishment.
Obtaining Necessary Permissions: Researchers need to obtain the appropriate authority before gathering data. IRB approval for human subjects research must also be obtained, as well as compliance with the necessary rules and regulations like GDPR and HIPAA for data protection.
Establishing File Naming Conventions: The consistent and organized file naming conventions that facilitate the traceability and organization of data are crucial. A naming convention should be set for files and folders for easy retrieval and clear understanding. Additionally, fine-grained descriptions should be provided for each dataset.
Implementing Storage and Backup Policies: The design of secure storage and backup policies is crucial in mitigating data loss. Researchers must determine the best storage platforms, whether secure servers or cloud-based and implement regular backups to prevent data loss through technical failures or information breaches.
Addressing Data Access and Sharing Considerations: Ethical issues related to research data access and sharing should also be included in the research. This includes assigning access permissions, determining which members can add or modify the data, and installing the insure security practices to protect confidential data. Furthermore, the protocol the researchers should establish for data sharing with other collaborators and compliance with the data-sharing policies from funding agencies or journals should be ensured.
Suggestions for Improving Data Testing
Developing a Comprehensive Test Plan: Researchers should launch an extensive test plan designing the aims, ways, and criteria of data testing. This plan must outline the realizable type of tests, the datasets to be analyzed, and the anticipated results.
Selecting Appropriate Testing Techniques: Scientists should select fit testing methods, considering the nature of the research data and those specific questions. Such statistical tests as chi-square tests, regression analysis, and hypothesis testing could be used if the variables to be studied would be specified.
Determining Sample Sizes: Without an adequate sample size, the results of our study will be statistically insignificant. Researchers have to base the sample sizes on statistical power analysis and consider the effect size, variability, and significance level, leading to more reliable findings.
Remaining Vigilant for Anomalies: Therefore, researchers need to be alert for deviations or strange occurrences during the experiment. This entails rigorous data input validation, flagging anomalies or inconsistencies, and timely action to correct data quality issues so as not to jeopardize the findings.
Research Limitations
Addressing the research limitations is key to accurately depicting the study results and their implications. Some of the critical research limitations include the following.
Hypothetical Nature of the Analysis: The hypothetical study may not adequately portray the practical results. It is essential to identify that the analysis to follow is speculative and will require further experimental research to confirm the hypotheses put forward.
Potential Biases in Hypothetical Scenarios: The simulation may be based on researchers’ prejudices or presumptions that, if left uncorrected, may affect the reliability of findings. It is vital to evaluate the study’s bias potential to determine its effectiveness and the results obtained after the study (Baldwin et al., 2022).
Assumptions Regarding Patient Demographics and Telemedicine Usage Patterns: The analysis uses patients’ demographics and telemedicine usage patterns as assumptions, but these may not match the real-world populations or practices. The populations might differ in real-world scenarios and hence provide unreliable conclusions.
By effectively considering the above limitations, it is essential to raise the study’s thoroughness and reliability. Maintaining the transparency necessary for carrying out the research and understanding the impact of telemedicine implementation in the healthcare sector is vital. This will provide a better understanding of the topic and enhance the base for its reliability in future studies.
Conclusion
Eventually, this fictional paper explains the possible effect of telemedicine on healthcare access and quality by revealing a few such impacts as patient satisfaction, clinical outcomes, and healthcare utilization. Even though the ANOVA test results showed that telemedicine implementation does not impact disease management significantly, it is important to discuss the study limitations, such as a hypothetical nature and assumptions about patients’ demographics and their usage frequency of telemedicine. The research advises maintaining robust research data management practices, understanding institutional policy relevant to the data research, obtaining necessary permissions, creating file name conventions, developing storage and backup policy, and taking data access and sharing into account. Looking ahead, it should be noted that the statements discussed here are speculative. Therefore, experimental studies that can prove the theories suggested and identify potential bias issues are needed. By overcoming the mentioned shortcomings and keeping the research practices upfront, we will better understand the influence of telemedicine implementation in the healthcare sector and contribute to more thorough case studies in the future.
References
Eze, N. D., Mateus, C., & Cravo Oliveira Hashiguchi, T. (2020). Telemedicine in the OECD: an umbrella review of clinical and cost-effectiveness, patient experience and implementation. PloS one, 15(8), e0237585.
Aashima, Nanda, M., & Sharma, R. (2021). A review of patient satisfaction and experience with telemedicine: a virtual solution during and beyond COVID-19 pandemic. Telemedicine and e-Health, 27(12), 1325-1331.
Merrill, C. B., Roe, J. M., Seely, K. D., & Brooks, B. (2022). Advanced telemedicine training and clinical outcomes in type II diabetes: a pilot study. Telemedicine Reports, 3(1), 15-23.
Baldwin, J. R., Pingault, J. B., Schoeler, T., Sallis, H. M., & Munafò, M. R. (2022). Protecting against researcher bias in secondary data analysis: challenges and potential solutions. European Journal of Epidemiology, 37(1), 1-10.
 write
write