Abstract
This research paper explores the effective approaches of treating and managing depression among adolescents in the United States. The paper applies a descriptive research design by reviewing the available literature to ascertain the effectiveness of the proposed treatment approaches to addressing depression among young people. Drawing on the available literature, depression is a significant public health issue among adolescents in the US and across the world. Depression and other mental-related disorders negatively affect individuals, their families, and society. Therefore, this calls for the need of various treatment approaches to manage the condition. Some of the effective methods discussed in this paper include psychotherapy and pharmacotherapy approaches. Psychotherapy approaches include the use of cognitive behavioral therapy (CBT) and interpersonal therapy (IPT), while in severe cases, there is a need for the combination of antidepressant medications and psychotherapy treatment approaches. However, these treatment plans have not been able to effectively manage depression among adolescents, thus calling for a review of these treatment approaches.
Keywords: depression, adolescents, psychotherapy, pharmacotherapy, depression management, mental health issues, cognitive behavioral therapy, interpersonal therapy, antidepressants
What are the most effective ways to treat depression in adolescents in the US?
Adolescence is one of the critical periods in a person’s life where they learn and develop different knowledge and skills. In the adolescent stage, young people develop skills on how to manage relationships and emotions as well as acquire some important abilities and attributes that are important in adulthood life. Depression is common among many adolescents, with a prevalence of about 4 to 5% as teenagers approach their mid and late adolescent years (Beirão et al., 2020). Adolescence is one mental health disorder that has an increased risk for suicide among adolescents and sometimes contributes to education and social impairments. Depression is the major chronic and debilitating condition in the United States, affecting between 12% and 25% of adolescents. Lewandowski et al. (2013) assert that the long-term prevalence of dysthymia and depression, which are common mental health disorders among the teens, usually increases from about 8.4 percent for the children aged between 13 to 14 years to about 15.4 percent for the teens aged between 17 to 18 years (Lewandowski et al., 2013). Development of depression before an individual reaches the age of 12 years has been regarded as the main cause of poor functioning and other long-term and repeated episodes of depressive disorders (DDs); comorbidity; suicide attempts, and other impacts that affect an individual’s wellbeing. Adolescent depression, which has been recording a rapid increase among young people, has been associated with negative health, social, and academic outcomes, including developing depression episodes in adulthood, contributing to indulgence in substance abuse, early pregnancies, and increased risks of suicide attempts. As a result, various treatment approaches have been developed to help manage the condition and ensure that the affected individuals attain healthy mental status. This paper will examine the most effective treatment approaches to managing depression among adolescents in the US.
Literature Review
According to Lewandowski et al. (2013), depression is one of the most disabling and prevalent mental health conditions due to educational and social dysfunctioning and emotional suffering. It is one common mental health disorder that affects many children, especially during their adolescent age. About 30 years ago, depression was considered a disorder that affected adults, with young people considered immature in developing depressive-related disorders. However, developmental studies have shown an increased occurrence of depressive disorders in recent years, especially among adolescents (Maughan et al., 2013). Depression, one of the major depressive disorders, results in severe effects in an individual’s life, especially when the condition develops in early childhood and adolescence. The rate of depression is attributed to an increase from childhood throughout adolescence and into adulthood, where severe consequences manifest. A study conducted Gunlicks-Stoessel et al. (2016) revealed that about 12.8% of the adolescents in the US aged between 12 and 17 years had reported symptoms of one or two DD episodes in 2016. About 8 percent of the population have attempted suicide in their lives, which makes depression one of the second leading causes of high mortality rates among teenagers between 12 and 17 years (Gunlicks-Stoessel et al., 2016). With the increased case of suicide cases among young people alongside the detrimental effects and consequences that depression causes to adolescents, several treatment interventions have been developed as a way of helping teenagers cope with their life situations and make informed decisions.
There are several risk factors accosted with depression among adolescents, including the social, psychological, and physical changes that occur during the adolescent stage, making the transition period a higher risk for developing depressive disorders. The symptoms are presented through the antagonistic behaviors and personality, which are the predictive symptoms of depression as presented in boys (Radovic et al., 2014). On the other hand, introspection and excessive feminine interaction role serve as the main characteristic of classifying the symptoms of depression among adolescent girls. However, compared to boys, girls in the adolescent stage are more likely to develop depressive disorders than boys due to the developmental aspects in their lives, which exacerbate their vulnerability; thus, fostering cognitive rumination and negativity. Radovic et al. (2014) asserts that the family environment is the major contributor to depression among teenagers due to the deprived family interactions, rejection conflicts, and physical and emotional abuse compared to the non-depressed adolescents. Children who have a history of maltreatment in their childhood are at a greater risk of developing depression and other depressive disorders than those without such a history (Nardi et al., 2013). Other personal attributes such as depressive attribution style, negative cognition, poor coping skills, reduced physical activities, use of tobacco and other substances, poor social competence, and physical illness have contributed to the development of depression.
The early intervention serves as the key ingredient to treating depressed adolescents in the community. These early interventions are made available in the major depressive disorder (MDD) pediatric treatment, which encompasses antidepressant medication and psychotherapy (Colizi et al., 2020). Some commonly used antidepressant medications among youths include selective serotonin reuptake inhibitors (SSRIs). Although there are instances whereby the risk of suicidal thoughts may increase with the intake of the depression antidepressant medication, the risk is higher with untreated depressive episodes (Mullen, 2018). Various treatment interventions have been tested and accredited in treating adolescents and older children. However, there are three main treatment options; evidence-based treatment recommended for treatment of depression among adolescents, which are in some instances used in treating adults but with lesser doses in children compared to adults (Salk et al., 2016). The first approach is the pharmacotherapy treatment used with fluoxetine. According to Lewondowski et al. (2013), antidepressants are not effective in children as they are in adults. The reasons behind this aspect have still not been unfolded. However, one of the antidepressants which have shown positive results among children is escitalopram in the US.
The second category of depression treatment among adolescents is cognitive-behavioral therapy (CBT) which has been widely recommended as the best treatment option for adolescents and children suffering from depression. Nations such as the UK consider CBT as the initial line of treatment for children suffering from mild depression episodes (Mullen, 2018). However, the evidence regarding the use of CBT alongside other medications such as fluoxetine is mixed. The last evidence-based treatment for depression is interpersonal therapy (IPT) which continues to garner increased acceptance and is widely used in different countries (Maughan et al., 2013). IPT has proved to be one of the most effective and useful treatment approaches among children suffering from depression. The provision of IPT, which takes place in the school settings and other settings, has proved to be effective in helping trace the root cause of the issue and helping the relevant healthcare professionals devise individualized plans for each patient (Thapar et al., 2010). Interpersonal therapy involves individual therapies, family therapies, and the involvement of other significant figures in the life of children, which will be beneficial in helping the child remodel their behavior and ability to cope with life stressors.
Methodology
Purpose of the Study
The main purpose of this study was to explore some of the proven and tested treatment options among adolescents in the US suffering from depression. Depression is one of the major public health issues affecting young people in the US and is one of the country’s most common types of mental health disorders. Although various interventions and treatment approaches have been developed, this study highlights some of the effective treatment options that have produced positive outcomes, especially when applied specifically to young people. Also, the study aims to provide future recommendations regarding some improvements required in terms of the integration of the treatment approaches to depression among teens.
Study Design and Instrument
The study adopted a descriptive research design. This is a research methodology that seeks to explore the available literature to systematically explain a phenomenon or explanation. This research was ideal for this study because it focused extensively on describing effective ways of treating depression among teens in the USA.
Study Population
The main study population in this project are adolescents aged between the ages of 10 to 19 years. This is one of the ages where children experience various depressive symptoms, which may be attributed to various factors, including their body changes as they prepare to shift from childhood to youth-hood.
Sample
Based on this target population, the researcher randomly selected a sample of adolescents from all states in the country, aged between the ages of 10 years to about 19 years. The researcher then compared the different rates of mental wellbeing among adolescents from different states against the types of interventions that different states use and the outcomes of these treatment approaches. The researcher also deployed an unspecified sample size because they overly depended on the available statistics on the national and government bodies and access the available healthcare facility statistics regarding the mental status of youths across the country.
Procedure
The researcher adopted both primary and secondary procedures of data collection. The primary method involved collecting first-hand information in the healthcare facilities from across all the states. On the other hand, the researcher reviewed the secondary data collection methods through a review of available literature. Collected data was then analyzed through statistical methods and interpreted to make meaning through qualitative and quantitative methods.
Ethical Implications of the Study Project
The researcher ensured that all the information collected from this research was only used for academic purposes and not any other aspects which may violate the academic research requirements. Also, following the institution’s requirements in conducting a research project, all available personal information of various patients in the target population was made confidential from third parties.
Results
From the review of the available information regarding the issue of depression among adolescents in the United States, various findings were drawn. Depression is one of the common types of depressive disorders among children and adolescents in the US. In the last 30 years, the rate of depression among young children has been steadily rising. In 2020 alone, it is estimated that about 4.1 million children aged between 12 and 17 years tested positive for one or more DD (NIH, 2022). This number represents about 17 % of the American population, a significant percentage of the American people who, if not treated, may prompt a larger American population consisting of mentally unstable individuals. The diagnosis of depression was higher among females than the male gender at 9.2% due to several reasons. As shown in figure 1 below, the rate of depression among the ethnic communities greatly differs, those with more than one race registering a higher prevalence of 29.9%.
Figure 1: prevalence of depressive disorders among adolescents
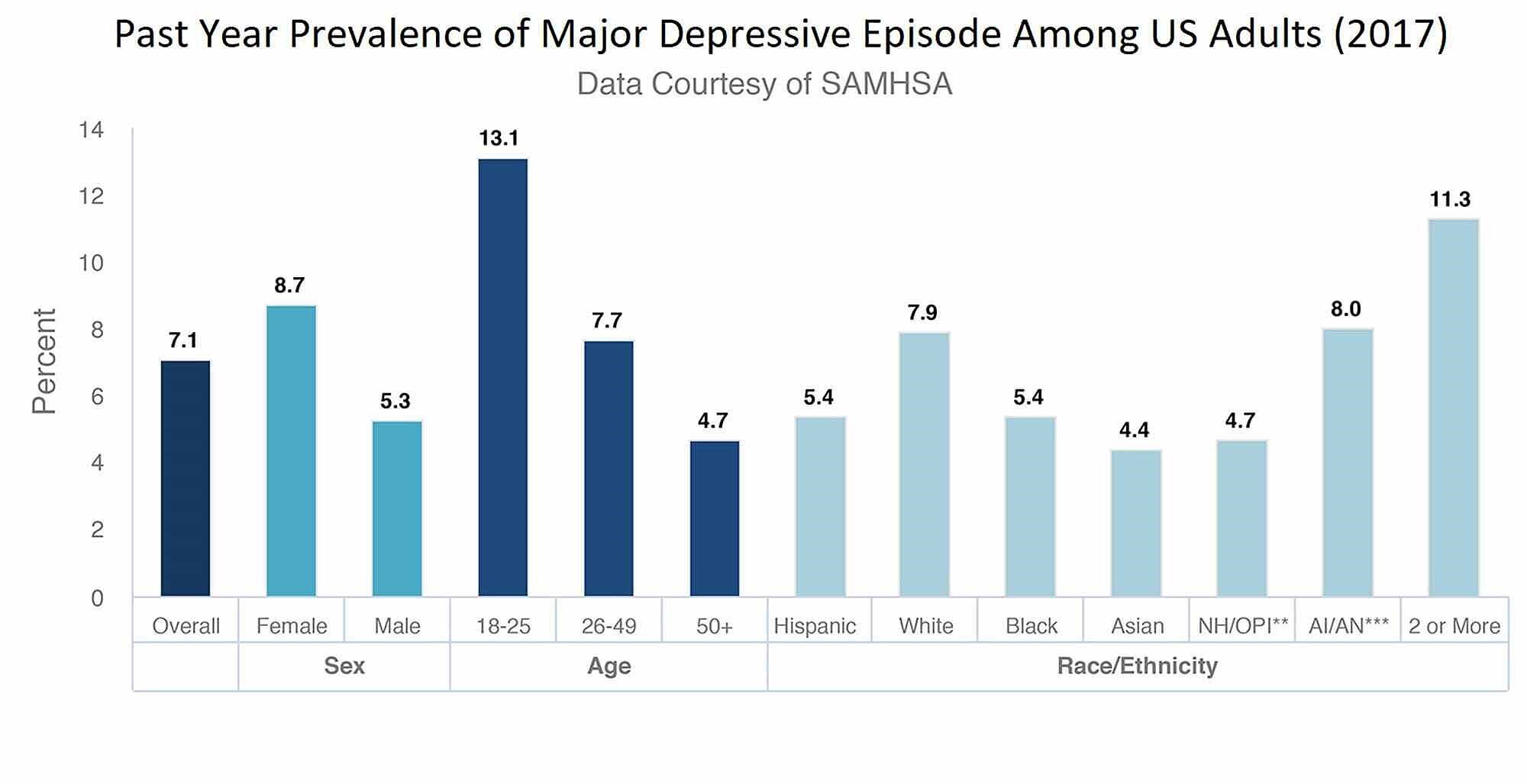
Source: NIH (2022)
Several factors cause depression among adolescents. These factors greatly contribute to the development of depressive behaviors, which range from the social, psychological, and physical changes, making the transitions by children during the adolescent stage risky to developing depressive disorders. Depression usually develops in different stages, with mild symptoms before puberty but later prolonged into adolescents, especially among young girls. Concurrent comorbidity alongside the disruptive emotional and disruptive disorder is usually common among adolescents, which are protracted through disruptive behaviors such as abuse of alcohol and other drugs. Adolescent-related impacts range from suicidal thoughts and attempts to poor mental and physical health, and social interaction and functioning difficulties. Exposure to stressful life events alongside the changes in familiar history contributes to the development of depression among teenagers. Children who underwent physical and emotionally abusive events, especially during their early childhood years, are three times more likely to develop depression than those who did not.
In the recent age, various interventions have been developed to help address the issue of depression among adolescents. The early intervention is one of the first and initial steps in addressing depression among adolescents, which is available in the pediatric segments of the healthcare facilities. Early interventions include early screening and diagnosis for adolescents who present themselves to hospital facilities for medical conditions other than mental health disorders. There are also evidence-based approaches that have proved effective in helping young teens adopt healthy behaviors and thus regain their normal mental health state. Depressed adolescents can benefit from the pharmacotherapy and physiotherapy treatment approaches which can either be used in individuals or combination with the antidepressant medication. However, applying these treatment approaches tends to affect depressive disorders moderately. CBT and IPT are some of the recommended treatment approaches to depression with a combination of antidepressant medications. The treatment approaches have their positive and negative effects on the children, and their reactions are different compared to when applied to adults.
Discussion and Conclusion
The main goal of this research project was to examine some of the available and effective treatment options devised to address depression among adolescents in the US. Depression is the most common type of mental health disorder affecting young people, especially adolescents. It is estimated that about 1.4 million cases of depression will be recorded among adolescents aged between 12 and 17 years in 2020 (NIH, 2022). This is a significant number, accounting for 17% of the American population. In the past three decades, depression has been considered an adult disorder, with studies indicating that the immaturity of children made it difficult for them to develop any related mental disorder. However, the current research has proved this assumption irrational. The recent years has been recording an increased rate of adolescents diagnosed and presenting depression-associated symptoms. From the review of the available literature, it is evident that compared to the male gender, young girls are at a greater risk of developing depression due to the dramatic changes taking place within their bodies. These changes usually compel the girls to behave in certain ways, which have also been attributed to their involvement in active sexual activities, leading to early pregnancies and an increased number of young mothers. Depression results in several harmful effects on its victims (Thapar et al., 2010). Some of the impacts of depression, especially when it begins before the age of 12 and prolongs into adulthood, include indulgent in drugs and substance abuse, development of antisocial behaviors, difficulties in forming and maintaining relationships, poor academic performance, among other several consequences which include development of other depressive mental disorders.
As a result of the increased need to address the high number of children suffering from depression, various treatment interventions have been developed. The first approach involves early interventions, which are significant in detecting earlier symptoms before they develop into full-brown symptoms, which are usually difficult to treat. Early interventions are the primary management tool that many pediatric departments use in ascertaining the mental status of children and adolescents visiting healthcare facilities for other medical conditions (Lewandowski et al., 2013). The treatment options among the pediatrics where the adolescents are classified vary in severity of the condition compared to adult treatment approaches. In individuals suffering from moderate or mild depression levels, the most effective approach to addressing their condition involves the use of psychotherapeutic methods, including psychoeducation where family members and other significant figures can be involved. With education, the affected individual can understand and track the root cause of their problems, thus increasing adherence to the treatment goals and plan.
On the other hand, in some situations, the healthcare providers may suggest using the two significant psychotherapeutic approaches; CBT and IPT. In severe cases, there is a need to combine the psychotherapeutic approaches with the pharmacotherapy approaches, which involve medications. Pharmacotherapy treatment comprises the administration of antidepressant medications, regarded as the first-line response of treatment in moderate to severe symptom presenting cases (Colizzi & Ruggeri, 2020). Antidepressants are usually provided to patients who fail to yield positive results using randomized and controlled psychotherapy trials. However, antidepressants are not recommended when used in isolation as the only method of treatment, especially among pediatric patients, due to the negative effects that the medications may have on the children. Instead, it is advocated for the combination of these medications with psychotherapy. The main reason for the mix of methods is to avoid other negative contributions of the medication by increasing the risk of harm to the individual and those around them, especially regarding suicidal attempts. SSRIs serves as the first-line antidepressant agent commonly used to treat depression among adolescents, while fluoxetine is used for children aged 8 year and above, with escitalopram approved for children of all ages. However, among all the antidepressants, fluoxetine has been proved to have a significant effect in addressing depression symptoms among adolescents compared to the other antidepressant. However, there is a need for the clinicians and the health professional involved in addressing the issue of mental health issues among children to come up with more profound treatment approaches that effectively address this issue. This is due to the limitation and weaknesses of the available treatment approaches.
References
Beirão, D., Monte, H., Amaral, M., Longras, A., Matos, C., & Villas-Boas, F. (2020). Depression in adolescence: a review. Middle East current psychiatry, 27(1), 1-9.
Colizzi, M., Lasalvia, A., & Ruggeri, M. (2020). Prevention and early intervention in youth mental health: is it time for a multidisciplinary and trans-diagnostic model for care? International Journal of Mental Health Systems, 14(1), 1-14.
Gunlicks-Stoessel, M., Mufson, L., Westervelt, A., Almirall, D., & Murphy, S. (2016). A pilot SMART for developing an adaptive treatment strategy for adolescent depression. Journal of Clinical Child & Adolescent Psychology, 45(4), 480-494.
Lewandowski, R. E., Acri, M. C., Hoagwood, K. E., Olfson, M., Clarke, G., Gardner, W., … & Horwitz, S. M. (2013). Evidence for the management of adolescent depression. Pediatrics, 132(4), e996-e1009.
Maughan, B., Collishaw, S., & Stringaris, A. (2013). Depression in childhood and adolescence. Journal of the Canadian Academy of Child and Adolescent Psychiatry, 22(1), 35.
Mullen, S. (2018). Major depressive disorder in children and adolescents. Mental Health Clinician, 8(6), 275-283.
Nardi, B., Francesconi, G., Catena-Dell’osso, M., & Bellantuono, C. (2013). Adolescent depression: clinical features and therapeutic strategies. Eur Rev Med Pharmacol Sci, 17(11), 1546-1551.
NIH. (2022). Major depression. Available at: https://www.nimh.nih.gov/health/statistics/major-depression#:~:text=An%20estimated%204.1%20million%20adolescents,compared%20to%20males%20(9.2%25).
Radovic, A., Farris, C., Reynolds, K., Reis, E. C., Miller, E., & Stein, B. D. (2014). Primary care providers’ initial treatment decisions and antidepressant prescribing for adolescent depression. Journal of developmental and behavioral pediatrics: JDBP, 35(1), 28.
Salk, R. H., Petersen, J. L., Abramson, L. Y., & Hyde, J. S. (2016). The contemporary face of gender differences and similarities in depression throughout adolescence: Development and chronicity. Journal of affective disorders, 205, 28-35.
Thapar, A., Collishaw, S., Potter, R., & Thapar, A. K. (2010). Managing and preventing depression in adolescents. BMJ, 340.
 write
write