Introduction
This paper explains psychosocial support and its implications for mental health and health professionals throughout the system levels and in different circumstances. By evaluating the spectrum of implementations that have emerged in the recent literature On the Australian Aboriginal people, one-third of nursing home patients experience depression. Depressive disorders may vary in severity from slight to severe, and they can strike at any point during a resident’s stay in a nursing home. Patients who are admitted as elderly residents are times as likely twice as likely to die within twelve months of admittance, according to evidence. They have a larger functional impairment, require 7 percentage points more employees’ time. Outpatient appointments, pharmaceutical costs, and laboratory fees are all higher for older persons with depression. Terms and conditions stipulated have been presented as a way to improve this majority’s clinical treatment of depression. Several government and commercial organizations have developed their own set of standards and suggestions.
Developing nursing intervention for major depression:
Major depressive disorders is grouped under temperament issues which are portrayed by disturbances in the function of mindset, conduct, and influence that go past the ordinary vacillations that the vast majority experience (Tuominen et al, 2019). Nursing care plans objective for patients with significant depression incorporate deciding a level of debilitation, surveying the client’s adapting capacities, helping the client to manage what is going on, accommodating gathering mental requirements, and advancing wellbeing and health. Aboriginal Australians are viewed as at an especially high risk of mental sicknesses, for example, significant misery prompting self-damage and suicide are higher. Public information proposes that Aboriginal individuals are bound to be hospitalized for or die from mental and conduct problems than non-Aboriginals.
There are many difficulties looked at by mental health nurses who are really focusing on Aboriginal Australian people groups in psychological well-being services. One of these is that there is a shortage of data related explicitly to the area of mental well-being nursing and Aboriginal and Torres Strait Islander people groups and their variety of characters. Proficient practice with Aboriginal people groups is affected by the nurse’s mentalities and understandings (Ichinose & Fong,2020). The default activity by open public mental health services to accomplish this, conventional compulsory preparation connected with the wide area of Indigenous wellbeing and health services needs, doesn’t seem to advance into informed expert mental health practice for Aboriginal and Torres Strait Islander people groups. The thinking behind the nurses keeping up with conventional ways to deal with mental health nursing was not verbalized by the members as an expectation to prohibit Aboriginal and Torres Strait Islander people groups or working in manners that they believed were inconvenient or disadvantageous to them (Jones et al,2018). Thus, often experienced nurses’ personal interpretation of the patient’s mental capacity act effectively for designing a good nursing intervention. Here is a culturally safe nursing intervention plan for a severely depressed patient with risk of self-harm:
Nursing assessment
Distinguish the degree of suicide precautionary measures required. In the event that there is a high risk, does a hospitalization need? Or on the other hand, assuming there is a generally safe, will the client be protected to return home with management from a relative or a companion? For instance, does the client:
- Concede past suicide endeavors.
- Misuse any substances.
- Have no companions
- Have any suicide plans.
- Therapeutic Interventions
- Urge clients to communicate sentiments (outrage, trouble, culpability) and think of elective ways of taking care of sensations of outrage and disappointment. Listen to their cultural views and show interest in their views(Rudman et al,2019).
- Contact the family, and set up for emergency directing. Actuate connections to self improvement gatherings.
- On the off chance that, hospitalized, follow unit conventions. Ask them if they are facing any issues in the hospital
- Execute a composed no-suicide contract.
Evidence-based Psychoeducation strategy for depressive illness:
Depression is the most prevalent psychological illness in patients, and it can vary from non-pathologic melancholy to clinical syndromes that cause significant discomfort and incapacity. More severe depressive symptoms are associated with longer hospital admissions, physical suffering, worse treatment compliance, reduced quality of life, higher desire for hastened death, and committed suicide, which are all clinical concerns (Maharaj et al, 2019). Psychoeducation offers immense potential for different kinds of infections and different life issues because of the adaptability of the idea, which incorporates both discouraged ailment explicit information and methods for overseeing related conditions.
The Evidence-Based Psychoeducational systems have been utilized to treat an assortment of discouraged messes, incorporate intense and perilous circumstances other than disease, as well as more constant ailments (Jones et al, 2018). These projects are intended to help people who are unwell, as well as their parental figures or accomplices, adapt to the physical and mental repercussions of ongoing and intense ailment. 96 ladies matured 30 to 55 who were ready for an elective hysterectomy were haphazardly allotted to one of two gatherings: individual psychoeducational discussions or sound controls in one of the cross-public preliminaries. The quantity of members, length, and seriousness of the intercession class were not uncovered, making it challenging to evaluate how well the instructive part of the psychoeducational mediation was connected with the mental methods.
Patient who sought compelling treatment, then again, experienced considerably less uneasiness and passionate pain, as well as higher treatment fulfillment, soon after medical procedure than those in the benchmark group (Curry and Meyer, 2020). There was no distinction between the two gatherings as far as post-medical procedure drug needs. Heftiness and vague torment were the subjects of two different models that tended to persistent ailments. Critical thinking and self-assuredness preparing were stressed, as well as the etiology, dangers, and benefits, as well as the connection between self-perception and confidence. Psychoeducational members showed essentially more noteworthy confidence, body fulfillment, and more confined eating exercises following treatment as experienced by patients in the other two gatherings. The training just mediation members had comparable outcomes to the benchmark group. Persistent burdensome sickness has been associated with burdensome side effects like despairing, horrendousness, and sadness, as well as execution issues in the two people and families.
All in all, this investigation shows that psychological instructive nursing treatments have been utilized in an assortment of circumstances and at many degrees of government, but just those focusing on burdensome sickness can be considered proof based right now. Psychoeducational treatments give off an impression of being adequately versatile to stay away from a portion of the dangers. They’ve been used effectively as a head or advantageous treatment as a feature of an essential avoidance program up to this point. Research expected to assess the impacts of mediations on results across periods and in an assortment of circumstances is vital to more readily lay out viability and adequacy.
By connecting with and reinforcing both institutional and unconstrained emotionally supportive networks, psychosocial mediations can draw out the impact of treatment a long ways past the prompt situation. Psychological well-being intercessions have numerous executions for sickness and incapacity as well as different troubles in life all through levels of the general wellbeing, political and local area help, or potentially schooling area whenever planned and carried out insightfully, having observed indicated rules for conveying as well as depicting proof based psychoeducational methodologies.
Depression is a worldwide mental health issue. As a result, mental health providers must design evidence-based and cost-effective therapies. Psychoeducation is one of the psychosocial therapies (Reins et al, 2019). However, a recent Google search on the efficacy of psychoeducation for depression yielded mixed findings, necessitating a review of papers to determine the usefulness of psychoeducation. Ensure the efficacy of Evidence-based psychoeducation. The systematic review’ purpose is to look at the overall performance of psychoeducation for depression in randomised controlled trials (RCTs).
The Evidence-Based Psychoeducational technique is deemed essential in the therapy of major depressive illness. Despite this, a considerable percentage of patients do not react well to medication-only therapy, with high rates of relapse and recurrence. As a result, psychosocial therapies such as psychoeducation, as well as pharmaceutical techniques, have become increasingly acknowledged as critical components in the treatment of depression (Dedert et al, 2020). The goal of this systematic review was to examine the performance of psychoeducation for single phase depression patients.
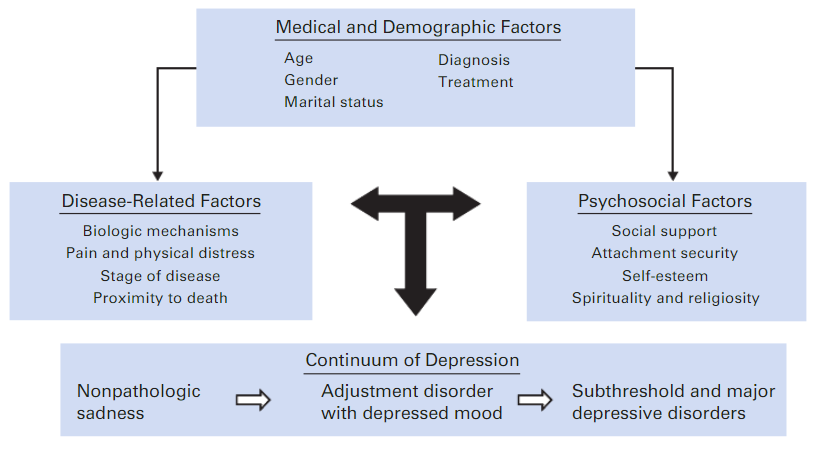
Figure 1: Depression’s Pathway
(Source: Jones et al, 2018)
Psychoeducation has proven to be one of the most successful evidence-based strategies in both clinical trials and community settings. Psychoeducation offers vast potential for various types of diseases and different life issues due to the flexibility of the concept, which integrates both depressed illness-specific knowledge and techniques for managing associated conditions.
The Evidence-Based Psychoeducational strategies have been used to treat a variety of depressed disorders, include acute and life-threatening conditions other than cancer, as well as more chronic illnesses (Jones et al, 2018). These programmes are meant to help persons who are unwell, as well as their caregivers or partners, cope with the physical and mental repercussions of chronic and acute illness. 96 women aged 30 to 55 who were prepared for an elective hysterectomy were randomly allocated to one of two groups: individual psychoeducational conversations or healthy controls in one of the cross-national trials. The number of participants, length, and severity of the intervention class were not disclosed, making it difficult to assess how well the educational component of the psychoeducational intervention was linked with the cognitive techniques.
Patient who got effective therapy, on the other hand, experienced much less anxiety and emotional distress, as well as higher treatment satisfaction, in the days following surgery than those in the control group (Curry & Meyer, 2020). There was no difference between the two groups in terms of post-surgery medication needs. Obesity and nonspecific pain were the subjects of two other models that addressed chronic medical conditions. Problem-solving and assertiveness training were emphasised, as well as the aetiology, risks, and advantages, as well as the relationship between body image and self-esteem. Psychoeducational participants showed significantly greater self-esteem, body satisfaction, and more restricted eating activities immediately after therapy as experienced by patients in the other two groups. The education-only intervention participants had similar results to the control group. Unceasing depressive illness has been connected to depressive symptoms such as melancholy, hopelessness, and despair, as well as performance issues in both individuals and families.
Conclusion:
In conclusion, this analysis shows that mental educational nursing therapies have been used in a variety of situations and at many levels of government, however only those targeting depressive illness can be deemed evidence-based at this time. Psychoeducational therapies appear to be adaptable enough to avoid some of the risks. They’ve been utilized successfully as a principal or supplementary treatment as part of a strategic prevention program so far. Research aimed to evaluate the effects of interventions on consequences across periods and in a variety of situations is crucial to better establish efficacy and effectiveness.
By engaging and strengthening both institutional and spontaneous support systems, psychosocial interventions have the ability to prolong the influence of treatment far beyond the immediate circumstance. Mental health interventions have many implementations for illness and disability as well as other difficulties in life throughout levels of the public health, political and community assistance, and/or education sector if designed and implemented thoughtfully, having followed specified guidelines for having to deliver as well as describing evidence-based psychoeducational strategies.
References
Tuominen, L., Stolt, M., Meretoja, R. and Leino‐Kilpi, H., 2019. Effectiveness of nursing interventions among patients with cancer: an overview of systematic reviews. Journal of clinical nursing, 28(13-14), pp.2401-2419.
Retrieved from: https://onlinelibrary.wiley.com/doi/abs/10.1111/jocn.14762
Ichinose, A., & Fong, Y. Y. D. (2020). Nursing Interventions on Adolescent and Childhood Depression in Primary Care: A Literature Review.
Retrieved from: https://www.theseus.fi/handle/10024/355286
Jones, R. B., Thapar, A., Stone, Z., Thapar, A., Jones, I., Smith, D., & Simpson, S. (2018). Psychoeducational interventions in adolescent depression: a systematic review. Patient Education and Counseling, 101(5), 804-816.
Retrieved from: https://www.sciencedirect.com/science/article/pii/S0738399117305918
Michaelis, R., Tang, V., Goldstein, L. H., Reuber, M., LaFrance Jr, W. C., Lundgren, T., … & Wagner, J. L. (2018). Psychological treatments for adults and children with epilepsy: Evidence‐based recommendations by the International League Against Epilepsy Psychology Task Force. Epilepsia, 59(7), 1282-1302.
Retrieved from: https://onlinelibrary.wiley.com/doi/abs/10.1111/epi.14444
Gladstone, T. R., Rintell, L. S., Buchholz, K. R., & Myers, T. L. (2021). Adaptation of an Evidence-Based Online Depression Prevention Intervention for College Students: Intervention Development and Pilot Study Results. Social Sciences, 10(10), 398.
Retrieved from: https://www.mdpi.com/1316140
Reins, J. A., Boß, L., Lehr, D., Berking, M., & Ebert, D. D. (2019). The more I got, the less I need? Efficacy of Internet-based guided self-help compared to online psychoeducation for major depressive disorder. Journal of affective disorders, 246, 695-705.
Retrieved from: https://www.sciencedirect.com/science/article/pii/S0165032718311121
Dedert, E. A., LoSavio, S. T., Wells, S. Y., Steel, A. L., Reinhardt, K., Deming, C. A., … & Clancy, C. P. (2020). Clinical effectiveness study of a treatment to prepare for trauma-focused evidence-based psychotherapies at a veterans affairs specialty posttraumatic stress disorder clinic. Psychological Services.
Retrieved from: https://psycnet.apa.org/record/2020-63303-001
Jones, R. B., Thapar, A., Rice, F., Beeching, H., Cichosz, R., Mars, B., … & Simpson, S. A. (2018). A web-based psychoeducational intervention for adolescent depression: design and development of MoodHwb. JMIR mental health, 5(1), e8894.
Retrieved from: https://mental.jmir.org/2018/1/e13
Curry, J. F., & Meyer, A. E. (2020). Evidence-based psychosocial treatments of depression in adolescents. In Handbook of evidence-based therapies for children and adolescents (pp. 121-136). Springer, Cham.
Retrieved from: https://link.springer.com/chapter/10.1007/978-3-030-44226-2_9
Maharaj, S., Lees, T., & Lal, S. (2019). Prevalence and risk factors of depression, anxiety, and stress in a cohort of Australian nurses. International journal of environmental research and public health, 16(1), 61.
Retrieved from: https://www.mdpi.com/386816
Rudman, A., Arborelius, L., Dahlgren, A., Finnes, A. and Gustavsson, P., 2020. Consequences of early career nurse burnout: a prospective long-term follow-up on cognitive functions, depressive symptoms, and insomnia. EClinicalMedicine, 27, p.100565.
Retrieved from: https://www.sciencedirect.com/science/article/pii/S2589537020303096
 write
write