Prevention of HIV among the African American Population In Georgia
African American People account for a higher proportion of people living with HIV and new HIV diagnoses as compared to other ethnicities and races in the U.S. In Georgia, HIV remains disproportionally Black. The gap in testing and treatment is attributed to stigma, substance abuse, and lack of insurance; even after the long periods of public health campaigns to cope with the virus, Black Georgians, specifically those living in Metro Atlanta, still make up a high percentage of HIV infections in the state in a disproportional rate. According to the Georgia Department of Public Health, although African Americans also made up 32 % of the state population, 71% of the 2500 Georgians were diagnosed with the virus in 2019 (Georgia Department of Public Health, 2021). Hence, a policy change is necessary to promote HIV prevention.
Barriers such as poverty, systemic inequalities, residential segregation and social and economic marginalization, homophobia, HIV stigma, and racism are among the longstanding barriers to health equality among Black or African American communities (“HIV and Black/African American people in the U.S.,” 2022). These barriers create profound negative impacts which are pervasive and deeply embedded in society hence affecting where a person plays, worships, works, learns, and lives and further inequalities in access to employment, wealth, quality education and housing, and other social and economic benefits (Nosyk et al., 2020).
The CDC estimates that in 2019, 1.2 million people were living with HIV nationwide. Blacks accounted for only 13% of the population in the USA but 40% of the people living with HIV (Fauci et al., 2019). The COVID-19 pandemic in America led to a disruption in access to clinical services and HIV testing all through 2020. The full impact of COVID will be known later on, but the recent CDC data has shown concerns relating to the setbacks in preventing HIV. These include slowed pre-exposure prophylaxis (PrEP) prescriptions and a sharp decline in HIV diagnosis and testing (Yancy, 2020). According to the CDC, in 2020, there were 44% fewer HIV tests administered among Blacks in non-healthcare settings as compared to 2019 (“HIV and African American people,” 2022). With the pandemic disrupting clinical care services and testing for new HIV infections, the CDC cannot estimate the number of new HIV infections.
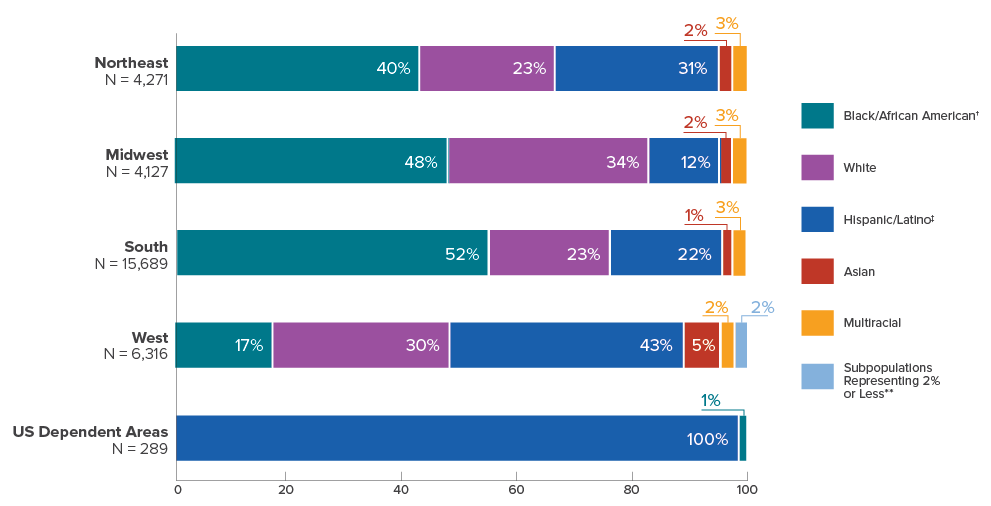
The disproportionality among the statistics is prominent not only among adults but also in children and infants. It is estimated that A.A. children were three times more likely to be perinatally infected with HIV than the total population. The disparity continues to rise among A.A. while that of the other racial counterparts has decreased within the decade.
The critical issue remains the HIV crisis in the African American (A.A.) setting. The risk factors associated with the high disparity rates in men are attributed to a combination of intravenous drug usage and men that have sex in men. In women, heterosexual contact is the highest risk factor for HIV infection. HIV/AIDS is a myriad of health issues that affect A.A. negatively. Significant health disparities exist within the community in rates of other issues such as cardiovascular diseases, cancers, and sexually transmitted infections. These disparities are fundamentally caused by structural and social factors, including racism, lack of access to dental and medical care, unrelenting stress, high incarceration rates, limited education opportunities, and attainment and poverty (Egede et al., 2020). Hence, the best plan of action to tackle the AIDS pandemic in Georgia is a state prevention approach integrated into nature that deals with the structural, social, and contextual environments that cause health disadvantages among African Americans.
Policy Recommendation
Georgia should allocate more funding and resources to the prevention of the virus, significantly because the unavailability of access to HIV testing and healthcare, as well as cultural AIDS stigma, has increased the rate or delay of treatment and diagnosis within the A.A. population (Airhihenbuwa et al., 2018). Georgia state legislators should pass a bill that supports resources and funding on a mission to rid AIDS among the A.A. community through healthcare contracts, strategic partnerships, and a network of pharmacies. Resource allocation and funding will increase access to treatment upon diagnosis, help save the state money, and reduce death and stigma through mass media awareness. Strategic campaigns to increase testing, abstinence, and pre-and post-exposure prophylaxis access. Effective prevention measures will align with the National HIV/AIDS strategy goals including; prevention of new HIV infections, Improving HIV-related health outcomes of people with HIV, reduce HIV related health inequalities and disparities, and attaining coordinated efforts that address the HIV epidemic among stakeholders and partners (“National HIV/AIDS strategy 2022-2025 (NHAS),” n.d.)
In addition, this policy would help address the structural and social environment as resources and funding would help create momentum among the medical professionals., leaders, the public health sector, and the community at large on reviewing the many factors responsible for the pandemic. Overall, the policy could help present the current primary status of HIV/AIDS and create a fundamental understating of the African American community’s issues. Adequate and appropriate resource allocation will help meet the community “where they are,” and this will help implement more culturally appropriate solutions as these have shown to be more efficient. This can help create health equality as all stakeholders, including public health practitioners, policymakers, community leaders, and the public health sector, may work towards assessing the stigma and access underlying the disease and encourage safe practices among the patient population.
A major Policy Alternative
A major policy alternative would be to address the socio-economic factors which affect the A.A. population. Social and economic status is a reliable and consistent predictor of many physical and psychological health outcomes. Socio-economic status is determined by economic and social factors such as place of residence, occupation, education, income, and ethnicity (“Economically disadvantaged | HIV by group | HIV/AIDS | CDC,” 2022). These factors are interrelated by factors of production as well as policies. However, a change in social and economic status cannot be done by one policy change and may not be effective as it is a long-term goal.
Conclusion
Expanding the prevention measures for the spread of HIV among the African American population will support the efforts towards achieving health equity among the disproportionate rates of Blacks in Georgia. HIV continues to be a national and international public health issue. It further causes health disparities in America, and everyone should be part of the solution to fight against the spread of HIV. The racial HIV and health gap is highly correlated with the racial wealth gap, a direct outcome of historical and systemic issues of segregation in employment, education, healthcare, and housing. These factors intersect with sexuality, gender, and poverty, among others, embody sexual exclusion and standard health inequalities. HIV/AIDS distribution indicates that race is a social index for impoverishment, isolation, and health inequalities.
The current health system was established when racial segregation and other forms of discrimination based on disability, sexual orientation, and gender identity were sanctioned by custom and law. This widespread discrimination led to structural health disparities for racial groups, which can only be solved through affirmative action. Even though racism is not loner the explicit discriminator, the legacy system still fosters some discriminatory practices as it has replaced the segregation language with new discriminators.
References
Airhihenbuwa, C. O., DiClemente, R. J., Wingood, G. M., & Lowe, A. (2018). HIV/AIDS education and prevention among African-Americans: a focus on culture. AIDS Education and Prevention.
Economically disadvantaged | HIV by group | HIV/AIDS | CDC. (2022, April 1). Centers for Disease Control and Prevention. https://www.cdc.gov/hiv/group/poverty.html
Egede, L. E., & Walker, R. J. (2020). Structural racism, social risk factors, and Covid-19—a dangerous convergence for Black Americans. New England Journal of Medicine, 383(12), e77.
Fauci, A. S., Redfield, R. R., Sigounas, G., Weahkee, M. D., & Giroir, B. P. (2019). Ending the HIV epidemic: a plan for the United States. Jama, 321(9), 844-845.
Georgia Department of Public Health, HIV/AIDS Epidemiology Section HIV Epidemiologic Profile, Georgia, 2021 https://dph.georgia.gov/epidemiology/georgias-hivaidsepidemiology-section/georgia-hiv-surveillance-data, Published September 2021, [Accessed: date]
HIV and African American people. (2022, June 28). Centers for Disease Control and Prevention. https://www.cdc.gov/hiv/group/racialethnic/africanamericans/index.html
HIV and Black/African American people in the U.S. (2022, August 25). Centers for Disease Control and Prevention. https://www.cdc.gov/nchhstp/newsroom/fact-sheets/hiv/black-african-american-factsheet.html
National HIV/AIDS strategy 2022-2025 (NHAS). (2022). HIV.gov. https://www.hiv.gov/federal-response/national-hiv-aids-strategy/national-hiv-aids-strategy-2022-2025/
Nosyk, B., Zang, X., Krebs, E., Enns, B., Min, J. E., Behrends, C. N., … & Montaner, J. (2020). Ending the HIV epidemic in the USA: an economic modeling study in six cities. The Lancet HIV, 7(7), e491-e503.
Yancy, C. W. (2020). COVID-19 and African Americans. Jama, 323(19), 1891-1892.
 write
write